Most payers struggle to manage and maintain provider data. On an average, 1 in 3 providers have a change in their information every year. Payers receive provider information from multiple sources – tracking and making appropriate updates to the provider master has always been a challenge. Industry spends over $2B every year on provider data and yet problems persist.
Bad provider data has significant costs to payers.

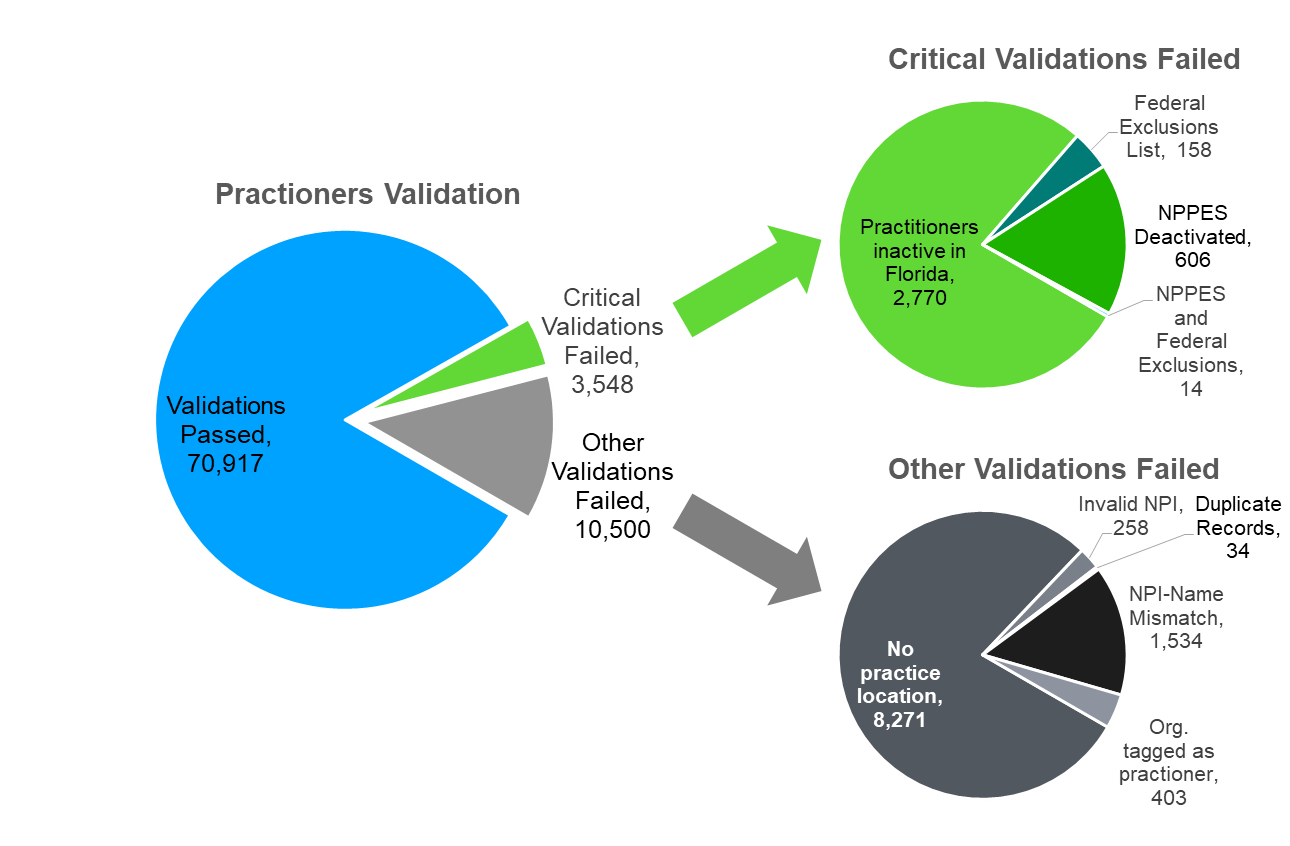
Health Sigma analyzed provider data for a regional FL payer with about 85,000 providers. Data quality assessment by Health Sigma identified that 4.2% of providers failed critical validations like inactive licenses, federal sanctions and NPPES issues. An additional 12.4% practitioners have other data integrity issues like invalid NPI, duplicate practitioners, NPI-Name mismatches and practitioners without a physical location.
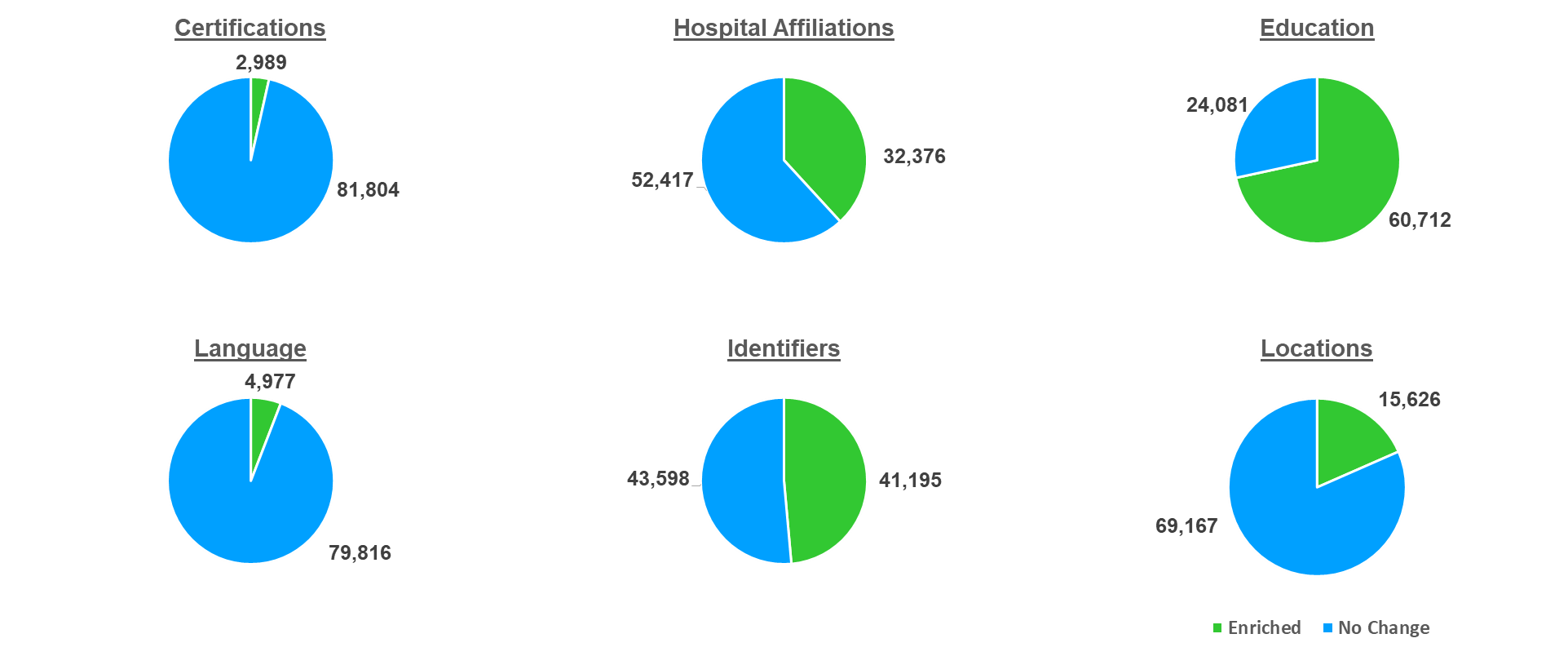
Apart from identifying issues in the provider data, Health Sigma enriched key information for providers leveraging automated data feeds from federal, state and other data sources